In my defense, there are two videos posted below. These are the first two EMS Week videos created by a department that is very near and dear to my heart. Watch....
“Always in Service”

May 21, 2017
EMS Week 2017 is upon us and as always there are a lot of positives that need to be pointed out. Its a time to recognize the little things that people do, and more importantly the people behind the uniform. It is the week of the year that should be about us, because the other 51 weeks out of the year should be about the patients that we serve. With taking all of that into consideration though, this is not going to be one of those positive posts. Last week, there was a call for articles and posts related to the tagline “EMS Strong: Always in Service” for this week’s message to providers. It asked for people to talk about what it means to them. Well, here you go. I grew up in a heavily volunteer driven community. When I started EMS, every BLS unit on the street was staffed by people dedicating their time. Much like myself, many went through their day to day activities with a Minitor II pager strapped to their hip, waiting to hear that rhythmic beeping that still gives me palpitations more than 20 years later. Day or night, weekend or weekday, on school vacations or snow days, it did not matter. I was always in service. At the time, I was a young, naive teenage EMT. I was happier on the ambulance than I was on the high school basketball court. I did not care if I got home from my summer job at 2am, if the pager went off at 3, I was going. I did not have a care in the world. EMS was what mattered to me. I was always in service. In college, I sacrificed many Friday or Saturday nights where my college friends would be out drinking and partying to throw on a uniform, turn on the radio and go trucking out of my dorm to take care of the sick, vomiting, and ETOH students of Springfield College. I cleaned vomit off of my boots. I cared for people that I might see in my economics class come Monday morning. I was ready to go at a second’s notice. I was always in...
The Ambulance of the Future

May 12, 2017
Roughly twelve years ago, AMR and AEV’s Safety Concept Vehicle made its way to Springfield for us to take a look at. It included a number of interesting features like an expanded harness setup to allow providers to move a little more freely around the box while still being anchored. There were mounting brackets for cardiac monitors, and video cameras to monitor both the rear of the truck for backing up, and the passenger side to check for traffic before opening the curbside door. The vehicle itself contained a lot of positives that have been adopted over the years. I see more cameras used in emergency vehicles and I’m a a fan of the checkered or striped patterns on the backs of trucks to make them more visible to oncoming traffic. I have also seen a few more monitor brackets. But where is everything else? When is that ambulance of the future going to get here? Year after year at conference after conference, there will undoubtedly be some ambulance parked on the exhibit hall floor touting itself as the “ambulance of the future.” Some have bucket seats that allow a treating paramedic to ride front facing with all equipment available at arm’s reach. Or cabinets replaced with pouches that can be slid on tracks to more easily make supplies accessible. Then, year after year, I pack up my chachkies and my six month supply of vendor provided pens and I head back to my EMS service relegated to sit on the same old bench seat that I sat on nearly 25 years ago when I first set foot on an ambulance that was ten years old at the inception of my career. I take the same risks while I care for my patients mainly because I have all but accepted the fact that if that ambulance is involved in a serious crash, I’m pretty much screwed anyway. Concept vehicles are great, but when is anyone going to do anything with them? I’ve worked in a just a couple of ambulances with the bench seat replaced by a bucket seat, and it left a lot to be desired. It felt cramped, and nothing like these...
Cross Promotion and CPR
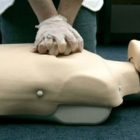
May 9, 2017
The biggest barrier to many systems’ CPR survival rates skyrocketing is the pubic’s lack of willingness to perform CPR before a rescuer gets on scene. Those roughly five minutes might be the most important five minutes in a patient’s chance for survival. Many systems have tried to teach more hands only CPR, or perform “flash mob” trainings as a way to get the word out there about the importance of CPR. Frequently, the top two concerns that I’ve heard expressed by the public are the perceived legal issues, or the “what if I do it wrong?” attitude, and the fear of giving mouth to mouth to a stranger. In reality though, neither of these factors truly come into play anymore with good Samaritan protecvtion laws and a new found focus on compression only CPR. This morning I read a news story shared by EMS1 about a woman who nearly lost her son who now hosts “CPR parties” and it got me thinking. My girlfriend has a problem, and I know that she is not alone. On an almost weekly basis, our mailbox becomes filled with products from some company called Lu La Roe, or as I have come to call it “Lou Lou La Rue.” In reality, I am okay with it because I feel a little more justified when I buy games off of Steam or have an afternoon of craft beer and Amazon Prime purchasing. She told me how she has spent time on Facebook attending virtual parties where people will go through their inventory on a platform like Facebook Live. I know for a fact that there are at least a couple of paramedics who sell products like Lu La Roe on the side, and I thought that this might be a great opportunity to do some teaching. In reality, all that one needs to learn how to do hands only CPR is a pillow and a couple of minutes. In corporate some “100 beats-per-minute” music, and a person could put together a free, informative CPR class that could save a life with just a couple of minutes of education tied in to a sales presentation. Seems simple, right? These are the...
An Apology to Those We’ve Lost
To expand on last week’s posts about the evolution of cardiac arrest, I got thinking about how things have changed over the centuries. I remember watching Killing Lincoln on the history channel a few years ago. In the moments after President Lincoln was shot, an army surgeon who was at Ford’s Theatre stepped up to care for the doctor. He instructed people to “lift his arms up and down” to help facilitate respirations for the president. Its something that today, we would look at as being ridiculous. The funny thing is, as I look over my career and a lot of the treatments that I talked about last week, I see a lot of what used to be cornerstones of resuscitation only a few decades ago as being equally as ridiculous. It makes me wonder how many life saving events that I could have been a part of had our approach to cardiac arrest been similar to what it is today. The changes that we have seen in the last 20 years have been simple ones. We have changed compression rates. We’ve prioritized compressions. We have realized that getting that tube is not nearly as vital as we once thought it was. 17 years ago, if I delivered a code without a tube to the ER, it was seen as a badge of shame. You did everything you had to do, the rest of the care be damned, and you got that tube. What if we had stayed on scene and played for some of those codes instead of just throwing a backboard under them and whisking them away to the hospital morgue? What if we had admitted defeat to a difficult tube and stuck with a BLS airway since that was working anyway? What if we had done compressions in between my stacked 200, 300, and 360 joule shocks? How many more lives would have been saved? The first CPR save pin that I ever received was when I was 16 years old. The patient was 80-something and she collapsed at home. 22 years ago, New Jersey was doing some things right. If we didnt get them back we did not go anywhere. This patient though,...
The Evolution of Cardiac Arrest Care
As we start to dive down the rabbit hole of what makes an effectively run cardiac arrest, it is important to understand the roots of what we are actually doing. Personally, I could go back some 23 years to 1993 when I received my first CPR card. I learned the importance of opening the airway. Looking, listening and feeling. If the patient was not breathing, and I could not give a rescue breath, I had to reposition the airway. Simply put, until the patient had a patient airway, and was effectively being ventilated or breathing on their own, not a single compression was done. If I had somebody with me, for every five compressions that were done, a ventilation was given. If it was just me, it would be 15:2. Sometimes I am amazed that we saved anyone at all following that. In the system that I started in, I feel like we were ahead of the curve. CPR calls were commonly not transported to the hospital. We would work them at home and leave them at home. Fast forward now seven years to my time as a paramedic student and my early days as a paramedic. Not much from that airway focus had changed. ROSC was rare. Survival to discharge was even more rare. Every workable cardiac arrest was transported to the hospital regardless of rhythm or downtime. The success and failure of the care provided rested on two factors: whether the patient was turned over to the emergency room staff intubated, and whether or not the call time was short. We would walk away from a code high fiving each other for delivering a dead body to the ER in 30 minutes or less, like we were some glorified Dominos delivery drivers. Throughout my career, my views on EMS and the impact that we have on the general public has swung to both ends of the spectrum. I’ve felt that we were completely necessary for the well being and survival of every single person that we encountered, and I’ve felt used and abused by the system. As I enter my 16th year as a paramedic though, I can without a doubt say...
Comfort in Change
One of the things that amazes me about this field is how tightly we hold on to our beliefs. It does not matter if it has to do with oxygen management or medication administration, or even C-Spine. People always seem to revert back to how they were taught the first time that they learned something presumably because it is uncomfortable. Maybe it is time to get comfortable with being uncomfortable. Make it is time to make change a way of life. It has been my experience that people seem to base a lot of decisions that they make off of one negative experience in their career over a more frequent positive one. We balk at giving pain medications to some patients because we believe that they are lying to us thanks to that one addict that we feel pulled a fast one on us in the early days in our career. Or we put the nitro aside on an inferior MI because this one time a medic that you met told you about a medic that they knew who dumped the pressure on a patient who then coded on them. The truth is though that the person in pain, regardless of their background, could benefit from that fentanyl, and chances are, that person having the MI will maintain their pressure and could greatly benefit from the treatment that you are so reluctant to give them. Or take response times as another example. Despite evidence to the contrary, and despite studies that have been conducted, there is little correlation between response times and mortality in a majority of the emergencies that we as EMS providers respond to. I happen to know of one rather large service that despite having an excellent ROSC rate they see a lower percentage of CPR saves in the more densely populated section of their service area with considerably lower response times than they do in the more suburban or rural areas. While the difference in miniscule, it is further proof that despite the fact that somebody gets on scene more quickly than in other areas, speed alone does not constitute more lives saved. I have always found the concept of...
Knee Jerk Management
Your department has a policy that they send two ambulances to reported cardiac arrests. On one particular busy night two of your trucks are dispatched to a person reportedly not breathing. The first truck gets on scene and finds a patient beyond help. Before they can cancel the second ambulance, they are involved in an intersection accident. In response to this incident the next morning your director releases a memo stating that second ambulances will no longer be dispatched to cardiac arrests. In a labor management meeting, an employee suggests development of an “emergency code” for field personnel to report to dispatch that they are in trouble to help activate a large law enforcement response to assist them at their location. Your boss says that this will not happen because they think field crews will abuse it. A week later, a paramedic is seriously assaulted by a psychiatric patient. The dispatcher on the other side of the radio was unable to make out their calls for help. Your boss then revisits the policy. Your division uses a non-disposable laryngoscope blades. A supervisor goes to your boss and suggests following the industry trend and shifting to disposable ones to reduce the risk of infection for patients. Your boss decides against this since your company has never been sued by someone receiving an infection from this means of transmission. You are convinced that the only way this policy will change is through some sort of tragedy. All three of these incidents are loosely based on actual events that I have either been part of or have heard about from friends of mine working in different systems throughout the United States. They are all evidence of the same though, change driven by catastrophe. We have all experienced it at some point in our career. We have all been sitting around in a conversation with our friends and coworkers and had somebody utter the words, “Nothing is going to change until somebody gets hurt.” Some of this attitude from leadership is because of a generalized disconnect from the field. Some of it is because of the kneejerk, reactive nature of EMS that seems to carry on with people...
